Filter
22 products
Type: Sphygmomanometer
Mercury-Free Manual BP Monitor with LCD Display
Type: Devices
Omron HBP-1320 Blood Pressure Monitor White
Type: Sphygmomanometer
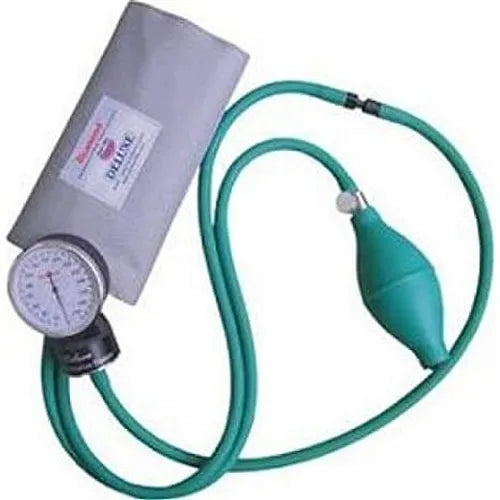
Diamond Dial Deluxe Sphygmomanometer with Field Calibration BP Apparatus
Type: Sphygmomanometer
Diamond Mercurial BP Instrument Stand Model with Velcro Cuff BPMR152
Type: Sphygmomanometer
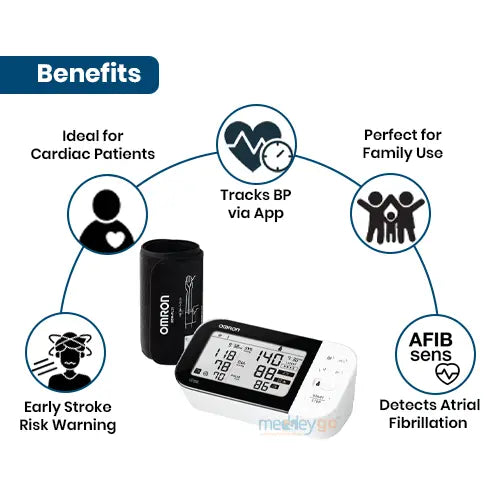
Omron HEM-7361T Bluetooth BP with AFIB Detection
Type: BP Monitor
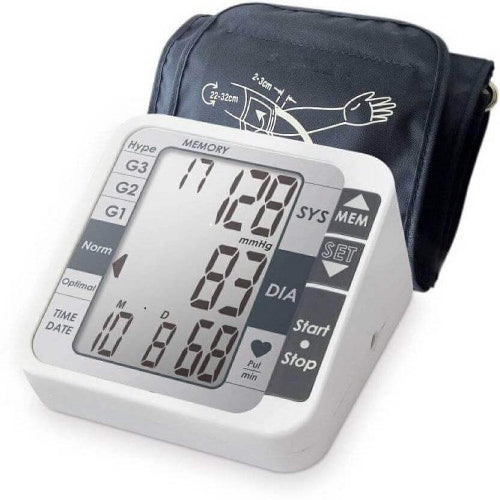
Desktop Blood Pressure Monitor Clock
Type: Sphygmomanometer
Mercury BP Monitor Mercury with Stand, For Clinic, 0-300mHg
Type: bpm
Beurer BM 81 Upper Arm Tubeless BPM with Easy Lock (BT)
Type: Home Healthcare
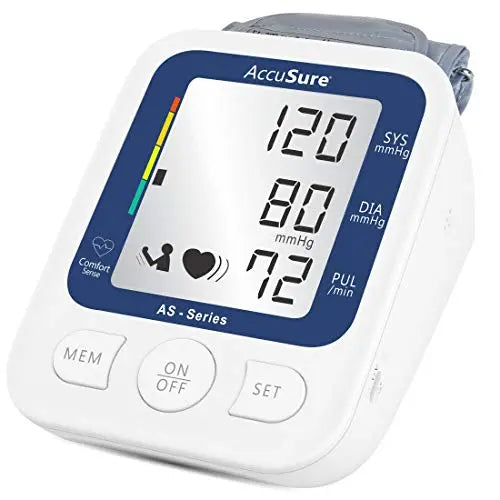
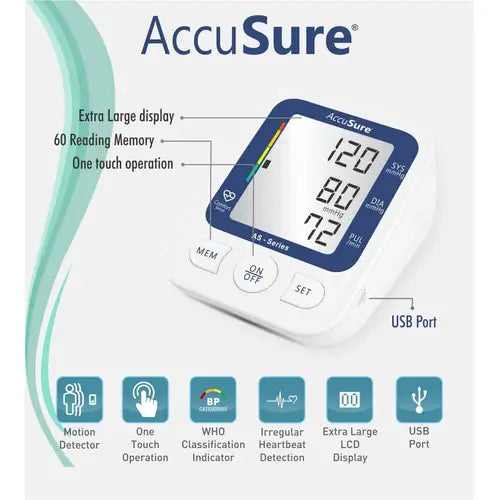
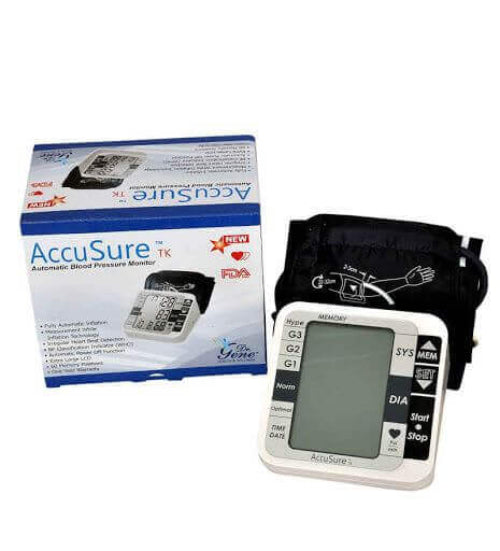
AccuSure AS Extra Large LCD and WHO Approved BP Machine
Type: Sphygmomanometer
Digital Blood Pressure Machine YE670AR
Type: Home Healthcare
AccuSure TS Smart Inflation BP Machine
Type: Sphygmomanometer
Digital BP Monitor Yuwell YE660F
Type: Home Healthcare
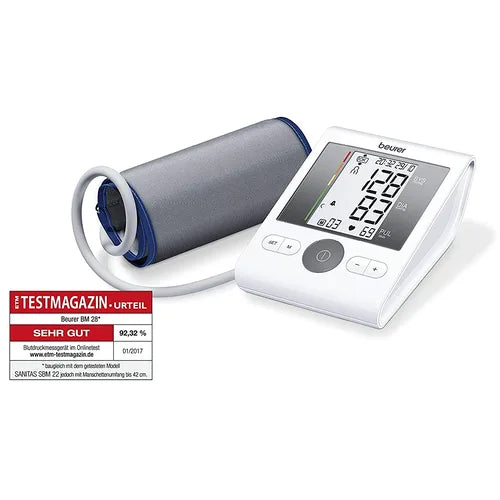
Beurer BM28 BP Machine with German Technology
Type: bp monitor
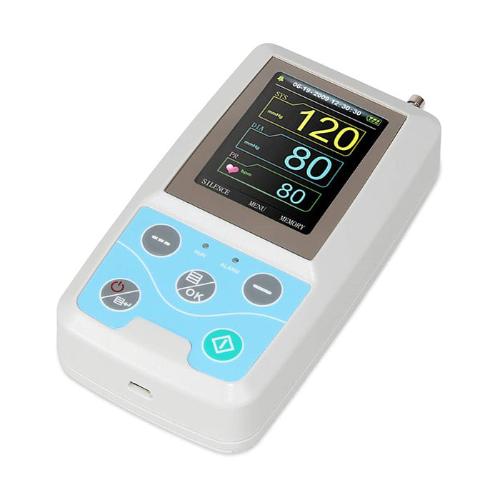
Ambulatory Blood Pressure Monitor with SpO2
Type: Sphygmomanometer
Beurer BM 96 Upper Arm BPM with ECG Stick (BT)
Collection:
Blood Pressure Guide: Levels, Control & Diet Tips
Understanding Blood Pressure: A Comprehensive Guide
120 over 80. You've probably heard that's the "golden number" for blood pressure. But what if your reading is 135 over 85? Or 115 over 75? Understanding your blood pressure isn't about memorizing perfect numbers---it's about learning to read the vital story they tell about your heart's health.
That familiar squeeze around your arm at the doctor's office often leaves you with numbers that can feel like a test you didn't study for. The real challenge is that high blood pressure typically has no symptoms. It can work silently in the background for years, which makes knowing your personal numbers one of the most important first steps you can take for your long-term well-being.
This guide translates those numbers into a clear story, breaking down what each one means and how to read a blood pressure chart without medical jargon. You'll get the simple, clear answers you need to feel confident and in control of this key part of your health.
Your Body's 'Plumbing': A Simple Guide to What Blood Pressure Is
You've had your blood pressure taken countless times, but what exactly is being measured? Blood pressure is the physical force your blood exerts on the inside of your artery walls as it travels from your heart to the rest of your body. It's a fundamental indicator of how hard your heart is working.
Think of your circulatory system like a garden hose: your blood vessels are the hose, and your blood is the water flowing through it. Blood pressure is simply the force of that water pushing against the sides of the hose.
This gentle force is vital. Without it, your blood couldn't circulate to deliver the oxygen and nutrients that your organs and tissues need to survive. A healthy amount of pressure ensures everything gets where it needs to go, keeping your body running smoothly. Too little pressure is a problem, but for most people, the concern is when the pressure is consistently too high.
The pressure inside your arteries isn't just one steady number. It rises and falls with every beat of your heart, which is why your reading always includes two numbers.
Decoding the Two Numbers: What 'Systolic' and 'Diastolic' Actually Mean
That blood pressure reading you get at the doctor's office always comes as a pair of numbers, like "120 over 80." These two numbers, known as your systolic and diastolic pressure, work together to provide a dynamic snapshot of the pressure inside your arteries. Each one tells a different part of the story.
The first, and higher, number is your systolic blood pressure. This measures the peak force on your artery walls at the exact moment your heart beats or contracts to pump blood out. Using our garden hose analogy, this is the maximum pressure when you turn the spigot on full blast. It reflects how hard your heart is working to push blood through your body.
After that powerful push, your heart needs a moment to relax and refill with blood before the next beat. The second, lower number is your diastolic blood pressure, which measures the force in your arteries during this resting period. In the hose, this would be the steady, constant pressure of the water between pulses. It shows how much tension your arteries are under when your heart isn't actively pushing.
Looking at both numbers reveals the full cycle of stress on your arteries. A high systolic number can indicate your heart is pumping with too much force, while a high diastolic number can mean your blood vessels aren't getting enough of a break between beats. Having this complete picture is the first step in understanding where your own numbers fall on the health chart.
From Normal to High: Finding Your Numbers on the Blood Pressure Chart
Now that you understand your two numbers, the next question is simple: are they healthy? While "120 over 80" is often called the gold standard, it's just one point on a wider spectrum. To help you see where you stand, doctors use a standard blood pressure chart with five clear categories.
To make sense of your own reading, find where your numbers fit in the levels below. The measurement "mmHg" simply means "millimeters of mercury," the standard unit for pressure.
- Normal: Less than 120/80 mmHg
- Elevated: 120--129 systolic and less than 80 diastolic
- High Blood Pressure (Hypertension) Stage 1: 130--139 systolic or 80--89 diastolic
- High Blood Pressure (Hypertension) Stage 2: 140 or higher systolic or 90 or higher diastolic
- Hypertensive Crisis: Higher than 180/120 mmHg. Seek immediate medical attention.
Pay special attention to the Elevated category. This range isn't considered high blood pressure yet, but it's a crucial warning sign. Think of it as a yellow traffic light---a signal to start making small, positive lifestyle changes to prevent your numbers from creeping higher. It's an opportunity to take control before a problem develops.
Once your readings consistently fall into Stage 1 or 2, a doctor will typically diagnose you with hypertension, the medical term for high blood pressure. This is the point where lifestyle changes become essential and medication may be discussed to protect your long-term health.
Most people in the elevated or even Stage 1 and 2 ranges feel perfectly fine. If there are no symptoms, why is it so important to get those numbers down? The answer lies in the slow, hidden damage it causes over time.
The Silent Damage: Why You Can't Feel High Blood Pressure
This lack of warning signs is precisely what makes high blood pressure, or hypertension, so dangerous. Unlike a headache or a fever, high blood pressure doesn't send out immediate alarms. Most people with hypertension feel completely normal, so they have no idea that a problem is quietly developing inside their bodies. This is why it has earned the ominous nickname the "silent killer."
To understand the damage, think back to our garden hose analogy. If you crank the water pressure up to its maximum and leave it on for years, the hose itself will start to suffer. Its flexible material will slowly become stiff, brittle, and develop weak spots. The same thing happens inside your body. Constant high pressure gradually damages the delicate lining of your arteries, making them less flexible and more narrow.
Over time, this wear and tear on your body's "plumbing" has serious consequences for the organs that depend on a healthy blood supply. Your heart is forced to pump much harder to push blood through stiffened vessels, leading to heart strain and failure. The fragile vessels in your brain can weaken, increasing the risk of a stroke, and your kidneys can lose their ability to filter waste from your blood effectively.
Because you can't rely on symptoms to alert you, the only way to know if you are at risk is through regular monitoring. Getting your blood pressure checked---whether at a doctor's office, a pharmacy, or with a home monitor---is the one and only way to catch this silent problem and take steps to protect your long-term health.
When the Pressure Drops: The Signs and Causes of Low Blood Pressure (Hypotension)
While most of the health conversation centers on high blood pressure, it's also possible for your numbers to be on the low side. This condition, known as hypotension, is the opposite of hypertension. For some people, especially young and active individuals, having consistently low blood pressure is perfectly normal and even a sign of good cardiovascular health.
The crucial difference is how you feel. Unlike high blood pressure, which is dangerous even when you feel fine, low blood pressure is generally only considered a problem if it causes noticeable symptoms. If your blood pressure is naturally low and you feel great, there's usually no reason for concern. The issue arises when the pressure drops enough to reduce the blood flow of oxygen and nutrients to your brain and other organs.
When this happens, your body will send clear warning signals. The most common symptoms of problematic hypotension include:
- Dizziness or lightheadedness, especially when standing up
- Fainting (syncope)
- Blurred vision
- Nausea
- Unusual fatigue or weakness
Several common situations can cause a temporary drop in blood pressure. Dehydration is a major culprit, as having less water in your body reduces your overall blood volume. Certain medications or even just standing up too quickly can also cause a brief dizzy spell. If you frequently experience these symptoms, it's a good idea to mention them to your doctor, who can help determine the cause. Tracking your numbers at home can provide valuable information for that conversation.
Get an Accurate Reading Every Time: How to Measure Your BP Correctly at Home
If you've decided to track your numbers with a home blood pressure monitor, getting a consistent and accurate reading is key. Your blood pressure isn't fixed; it can jump up if you've just run up the stairs or had a cup of coffee. To get a true picture of your health, it's crucial to measure your resting blood pressure.
Think of it as a mini-ritual. By following the same steps each time, you create a reliable log that you and your doctor can trust. For the most accurate results, health experts recommend this simple process:
- Relax First: Before you measure, sit quietly in a comfortable chair for five minutes. Avoid talking, scrolling on your phone, or watching an exciting TV show.
- Sit Properly: Your back should be supported, and your feet should be flat on the floor. Don't cross your legs, as this can temporarily raise your pressure.
- Position Your Arm: Rest your bare arm on a table or pillow so that the cuff is roughly at the same level as your heart.
- Take Multiple Readings: Press start. After the reading is done, wait one minute and then take it again. Taking two or three readings and averaging them gives a much more accurate result than a single measurement.
Following this routine ensures that you're not accidentally inflating your numbers due to activity or posture. A number taken while you're slouched on the sofa will be different from one taken while sitting correctly. Consistently capturing your true baseline pressure helps your doctor interpret your readings accurately.
Wrist vs. Upper Arm Cuffs: Which Blood Pressure Monitor Is Right for You?
When you start shopping for a home blood pressure monitor, the biggest choice you'll face is between a wrist vs upper arm cuff monitor. While both are available, there's a clear winner for accuracy and reliability: for most people, the traditional upper arm cuff is the better choice.
The reason is simple: your upper arm is a more direct and reliable place to measure blood flow from the heart. A standard blood pressure cuff fits snugly over this major artery, giving a reading that is less likely to be affected by your body position. This is why health organizations like the American Heart Association generally recommend them for home use.
Wrist monitors, on the other hand, can be tricky. Because the arteries in your wrist are smaller and not as deep, these devices are extremely sensitive to the position of your arm. If your wrist is even a little bit below the level of your heart, your reading can appear falsely high. If it's above your heart, it can seem falsely low. This precision is difficult to get right every single time, which can lead to confusing and inaccurate numbers.
For dependable results you can share with your doctor, investing in a "clinically validated" upper arm monitor is your best bet. "Validated" means the device has been tested against medical standards for accuracy. Brands like Omron offer widely trusted models that are easy to use, making an Omron blood pressure monitor a solid choice.
The Salt Connection: How a High-Sodium Diet Spikes Your Blood Pressure
When it comes to factors you can control, your diet plays a starring role in managing blood pressure. And within that diet, one of the biggest players is sodium---the main component of table salt. While a little is necessary for your body to function, most of us consume far more than we need, and this excess directly impacts the numbers you see on your monitor.
How does a sprinkle of salt on your food affect your circulation? Sodium acts like a magnet for water. When you eat a high-sodium meal, your body holds onto extra fluid to balance it out. This excess water increases the total volume of blood flowing through your blood vessels, which in turn raises the pressure against their walls. This is one of the most direct ways your diet can influence your readings.
Surprisingly, the salt shaker on your table is rarely the main problem. The vast majority of sodium in the average diet---over 70%---comes from processed and restaurant foods. It's hidden in things you might not even think of as "salty," like bread, breakfast cereals, canned soups, and salad dressings. This hidden sodium makes it easy to consume too much without even realizing it.
Becoming a "sodium detective" by reading nutrition labels is one of the most effective natural ways to lower hypertension. By simply comparing brands of your favorite foods, you can start making choices that support healthier blood pressure.
The Power of Your Plate: How the DASH Diet Naturally Lowers Blood Pressure
While cutting back on sodium is a crucial step, one of the most effective strategies for blood pressure control involves what you add to your diet. This is the idea behind a research-backed eating plan called the DASH diet. Standing for "Dietary Approaches to Stop Hypertension," this plan has been proven to be one of the best natural ways to lower blood pressure, often within just a few weeks.
The real power of the DASH diet comes from focusing on foods rich in minerals like potassium, calcium, and magnesium. Potassium, in particular, acts as a natural counterbalance to sodium. It not only helps your kidneys flush excess sodium from your system but also helps relax the walls of your blood vessels, easing the pressure inside. You're actively giving your body the tools it needs to maintain a healthy balance.
So, what does this diet look like on your plate? It's less about strict restriction and more about making simple, positive additions. The cornerstones of the DASH diet include:
- Plenty of fruits and vegetables
- Whole grains (like oatmeal, brown rice, and whole-wheat bread)
- Lean protein sources such as fish and poultry
- Low-fat dairy products
- Nuts, seeds, and beans
By shifting your focus to these whole foods, you naturally reduce your intake of the processed items where hidden sodium often lurks. Embracing the DASH diet is a powerful and sustainable way to take charge of your numbers. When this smart eating plan is combined with regular physical activity, the results for your heart can be even more impressive.
Move Your Way to a Lower BP: Simple Exercises That Strengthen Your Heart
Just as smart food choices can protect your heart, regular movement is one of the most powerful natural ways to lower hypertension. Think of your heart as any other muscle in your body. When you exercise, you're giving it a healthy workout. Over time, this makes your heart stronger and more efficient, so it doesn't have to work as hard to pump blood.
This newfound strength has a direct and beneficial effect on your blood pressure. A stronger heart can push out more blood with each beat. Because it accomplishes more with less effort, your heart can beat slower and less forcefully. As a result, the pressure on your artery walls decreases, which is how regular activity helps bring your numbers down into a healthier range.
So, how much movement is enough? Health experts agree on an achievable target: aim for at least 150 minutes of moderate-intensity activity per week. This isn't about running marathons; it's about activities like brisk walking, cycling on level ground, swimming, or even active gardening. You can break this goal down into smaller, more manageable chunks, such as five 30-minute walks throughout your work week.
Ultimately, the most important part of this journey is consistency. Even a 10-minute walk during your lunch break is a fantastic step that contributes to your weekly goal and reinforces a healthy habit. While building a stronger heart through smart eating and exercise is crucial, it's also important to address other lifestyle factors that can sabotage your progress.
Beyond the Plate: How Stress and Poor Sleep Sabotage Your Blood Pressure
Ever felt your heart pound when you're stuck in traffic or facing a tight deadline? That's your body's stress response in action, and it has a direct, immediate impact on your blood pressure. While a healthy diet and regular exercise are foundational, overlooking the effects of chronic stress and poor sleep can undermine your efforts. These invisible forces can keep your numbers stubbornly high, even when you're doing everything else right.
When you're stressed, your body releases hormones like adrenaline. This "fight or flight" alarm system tells your heart to beat faster and your blood vessels to narrow, causing a surge in your readings. While this is normal in the short term, the real problem begins when stress becomes constant. Your body never gets the "all-clear" signal, leaving your blood pressure elevated for long periods and straining your entire system.
Quality sleep offers the perfect antidote. Your blood pressure is meant to naturally fall while you sleep, giving your heart and blood vessels a much-needed break to rest and repair. When you consistently miss out on deep, restorative sleep, your body loses this critical downtime. This means your cardiovascular system stays under strain around the clock, a major obstacle to long-term blood pressure control.
Prioritizing relaxation and protecting your sleep, therefore, are not luxuries; they are essential for your heart's health.
A Two-Way Street: The Critical Link Between High Blood Pressure and Your Kidneys
That relentless pressure from within doesn't just affect your main arteries; it also places a heavy burden on hardworking organs like your kidneys. These incredible organs act as your body's master filtration system, cleaning your entire blood supply several times an hour. For this vital job, they rely on a dense network of tiny, delicate blood vessels.
Think of those tiny vessels as an extremely fine sieve. When blood flows through at a normal, healthy pressure, the system works perfectly. But chronic high blood pressure is like forcing water through that sieve with a firehose. Over time, the constant force scars and weakens these delicate vessels, making the kidneys less effective at filtering waste and excess fluid from your blood. This is how hypertension becomes a leading cause of kidney disease.
Here's where the problem becomes a dangerous two-way street. Healthy kidneys don't just filter blood; they also play a key role in regulating blood pressure. When they become damaged, they can no longer manage your body's fluid balance effectively. This causes your body to hold onto extra water, and they may also release hormones that drive your pressure even higher. Damaged kidneys can make your existing high blood pressure even worse.
This dangerous feedback loop is precisely why your doctor keeps a close eye on both your blood pressure readings and your kidney function. Interrupting the cycle is critical for protecting your long-term health.
Red Alert: When a High Reading Becomes a Medical Emergency
While high blood pressure usually works silently over years, some readings are an immediate red flag that you simply cannot ignore. Any blood pressure reading of 180/120 mmHg or higher is considered a hypertensive crisis. This is a critical level that requires prompt medical attention, as it puts a severe and unsustainable strain on your entire circulatory system.
A reading this high is serious, but it becomes a potential life-threatening emergency if it's accompanied by specific warning signs. These symptoms can indicate that the extreme pressure may be actively damaging organs like your brain, heart, or kidneys. Pay close attention if you or someone else experiences:
- Severe headache, often described as the "worst headache of your life"
- Shortness of breath
- Chest pain
- Sudden numbness, weakness, or tingling, especially on one side of the body
- Vision changes or difficulty speaking
If you have a reading of 180/120 mmHg or higher AND are experiencing any of those symptoms, do not wait. Call 911 immediately. It is crucial that you do not drive yourself to the hospital. Paramedics can begin life-saving care the moment they arrive.
Your Path to Control: A Simple Action Plan for Better Blood Pressure
The numbers from a blood pressure cuff are more than a verdict; they tell the story of your heart's health. By understanding the "why" behind them, you transform from a passive observer into an informed partner in your health, able to see not just the numbers, but the reasons they change.
Knowing what to do next is the key to lasting blood pressure control. The path forward doesn't have to be complicated. It rests on four simple pillars that help you manage your health effectively.
Your 4 Pillars of Control:
- Know Your Numbers: Measure your blood pressure regularly to understand your personal trends.
- Eat Smarter: Focus on whole foods and be mindful of sodium intake.
- Move More: Aim for a simple walk each day to keep your heart strong.
- Master Your Mindset: Manage stress and prioritize restful sleep.
You don't need to master all four pillars overnight. The journey to lower blood pressure starts with a single, manageable action. Don't try to do everything; just choose one. Success isn't about perfection, it's about starting. What is one small change you can commit to this week?
Think of your blood pressure not as a final grade, but as a dynamic guide. It's daily feedback that you can listen to and influence. With these simple tips, you are no longer just reading your health story---you are holding the pen.
Understanding the Importance of Blood Pressure Monitoring
Your doctor's blood pressure reading might be one of the least accurate snapshots of your true health—and that’s a key reason why monitoring it at home is so valuable. Between rushing to an appointment and the natural stress of a clinic, a single reading is often temporarily high. Health experts know that a clearer, more honest picture emerges when you can track your numbers in a calm, familiar setting, providing a true story of what your heart is doing day to day.
To make sense of those numbers, think of your arteries as a garden hose. The top number, called systolic pressure, measures the force when your heart beats and sends blood surging through your body; it's like turning the spigot on full blast. The bottom number, diastolic pressure, is the background pressure in your arteries when your heart rests between beats. This analogy provides a simple, practical way to understand blood pressure numbers.
Understanding systolic and diastolic readings is crucial because if that pressure stays too high for too long, it causes "wear and tear." Just as constant high pressure damages a hose, it can harden your arteries and force your heart to work overtime, leading to serious health risks down the road. The goal is to keep your numbers within a normal bp range, protecting your system from this silent, long-term strain.
Your 7-Step Checklist for a Perfect At-Home Reading
Ever check your blood pressure and get a number that seems way off, only to check it again a minute later and get a completely different result? This is a common frustration, but it’s often due to small, easy-to-fix details in your routine. To get a number you and your doctor can truly trust, consistency is everything. Following a simple pre-check ritual ensures that you are measuring your body’s true resting blood pressure, not just a reaction to your busy day.
Think of the following steps as your recipe for an accurate reading every single time.
Here is your foolproof checklist for how to correctly use a blood pressure cuff at home:
- Wait 30 Minutes: Avoid caffeine, exercise, and smoking for at least half an hour before you measure. These activities can temporarily spike your numbers.
- Rest First: Sit quietly in a comfortable chair for 5 minutes before you begin. No scrolling on your phone or watching an exciting TV show—just relax.
- Get Your Posture Right: Sit with your back straight and supported. Keep your feet flat on the floor and your legs uncrossed.
- Use the Bathroom: A full bladder can actually raise your blood pressure reading slightly, so be sure to go beforehand.
- Support Your Arm: Place your arm on a flat surface, like a table or armrest, so the cuff is roughly level with your heart. Your palm should be facing up.
- Place the Cuff on Bare Skin: Wrap the cuff snugly around your bare upper arm. It should be about one inch above the bend in your elbow.
- Take 2-3 Readings: Press start. After the reading is complete, wait one minute, then take it again. If you have time for a third, even better. The most accurate picture of your blood pressure isn't a single measurement—it's the average of these two or three readings.

Are You Making These 5 Common BP Monitoring Mistakes?
Following the 7-step checklist is the perfect foundation for an accurate reading. But sometimes, a few sneaky habits can still throw off your numbers, leading to a falsely high blood pressure reading and unnecessary worry. These small details are often the biggest factors that affect blood pressure readings at home, so learning to spot them is key to gaining confidence in your results.
To get the most trustworthy number, double-check that you are avoiding these five common mistakes when measuring blood pressure:
- Measuring over clothing. Even a thin sleeve can interfere with the cuff’s ability to get an accurate reading. Always place the cuff directly on your bare arm.
- Using the wrong size cuff. This is one of the most critical errors. The inflatable bladder inside the cuff should wrap around roughly 80% of your upper arm. If the cuff is too small, your reading will be artificially high; if it's too large, it may read too low.
- Talking during the measurement. Stay still and silent until the cuff fully deflates. Research shows that talking during a reading can temporarily increase your systolic pressure by 10 points or more!
- Letting your arm hang or holding it up. Your arm muscles have to work to hold a position, which can raise your reading. Always ensure your arm is relaxed and supported on a table or pillow at heart level.
- Checking right after a big meal or when you feel stressed. Digestion requires extra blood flow, and stress hormones cause a temporary spike. Give your body time to return to a true resting state before you measure.
By sidestepping these common pitfalls, you can be sure the numbers you log reflect your body at rest. This reliability also depends on the device you choose.
Arm vs. Wrist: How to Choose the Best Home Blood Pressure Machine for You
When it comes to choosing the best home blood pressure machine, the first decision you’ll face is often between an upper arm cuff and a smaller wrist monitor. While both are widely available, most health organizations, including the American Heart Association, recommend an automatic, cuff-style bicep monitor for the most reliable results. This isn’t just a matter of tradition; it’s based on simple physiology.
The main artery in your upper arm, the brachial artery, is a more direct and stable place to measure blood pressure. Because it’s closer to your heart and well-supported by the bone, readings taken here tend to be more consistent and less affected by small movements or changes in your body position. This is why your doctor or nurse almost always uses an upper arm cuff during your check-ups.
Wrist monitors, on the other hand, can be trickier to use correctly. Although convenient, the arteries in the wrist are narrower and not as deep, making readings more sensitive. For a wrist monitor to be accurate, your arm and wrist must be positioned perfectly at heart level throughout the entire measurement. Even a slight drop of your hand can cause a falsely high reading, while raising it too high can give a false low. This positioning challenge is the primary reason they are often less accurate for home use.
Regardless of the type you consider, the single most important factor is clinical validation. This means the device has been independently tested and proven to meet strict accuracy standards. Before you buy any ambulatory blood pressure device, look for phrases like “Clinically Validated for Accuracy” on the box or in the online description. This certification is your best guarantee that the numbers you see are trustworthy.

What's a 'Good' Number? Interpreting Your Blood Pressure Chart
Once you have your reading, the next step is understanding what it means for your health. Interpreting a blood pressure chart isn't about a single "good" or "bad" number, but about seeing where your average readings fall within established ranges. Health experts use five categories to assess blood pressure. Think of these as a guide to help you and your doctor decide on the best next steps for your heart health. Remember, only a healthcare professional can diagnose high blood pressure, but knowing these categories gives you the power to be an active partner in the conversation.
Here’s a breakdown of the adult blood pressure categories recommended by the American Heart Association and what is considered a normal bp range:
-
Normal: Below 120/80 mm Hg.
- What it means: Your blood pressure is in the ideal range. Keep up your healthy lifestyle!
-
Elevated: Systolic 120–129 and Diastolic less than 80 mm Hg.
- What it means: This is a heads-up. You're at risk for developing high blood pressure, making lifestyle changes more important than ever.
-
Hypertension Stage 1: Systolic 130–139 or Diastolic 80–89 mm Hg.
- What it means: Your doctor will likely recommend lifestyle changes and may consider medication based on your overall health risk.
-
Hypertension Stage 2: Systolic 140 or higher or Diastolic 90 or higher.
- What it means: Your doctor will almost certainly recommend a combination of medication and lifestyle changes.
-
Hypertensive Crisis: Systolic higher than 180 and/or Diastolic higher than 120.
- What it means: Seek immediate medical attention. These numbers indicate a potential for organ damage and should be treated as an emergency.
While these hypertension stages provide a clear snapshot, your blood pressure is a dynamic number. That's why consistent tracking over time gives a much more accurate picture than any single reading.
Why Keeping a Blood Pressure Log Is Your Most Powerful Health Tool
Understanding the blood pressure categories is a great start, but the real power comes from seeing the story your numbers tell over time. A single reading is just a snapshot, easily influenced by a rushed appointment or morning coffee. The true benefits of daily bp tracking emerge when you create a log, which is like a movie of your health. This movie allows you and your doctor to see trends, understand how your lifestyle affects your numbers, and make more informed decisions together.
Learning how to track blood pressure is surprisingly simple. All you need is a basic notebook and a pen. For each entry, just jot down the date, the time of day, your systolic (top) and diastolic (bottom) numbers, and a brief note about your activity. Did you just finish exercising? Were you feeling particularly stressed or relaxed? This context is incredibly valuable, helping to explain why a number might be higher or lower than usual on any given day.
To get you started on the right foot, we’ve made a simple guide you can use right away. You can download and print our free blood pressure log template to begin building a clear health record for your next doctor’s visit. This consistent tracking naturally leads to an important question: just how often should you be taking these measurements for the clearest picture?
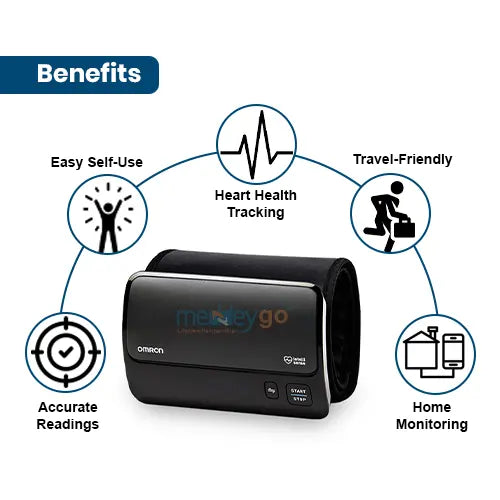
How Often Should You Take Your Blood Pressure for the Clearest Picture?
With your logbook ready, the next natural question is: how often should you take your blood pressure? While it’s tempting to check it constantly, the right frequency depends entirely on your goal. The answer for someone just diagnosed with high blood pressure is different from that of someone who has their numbers well-managed. The key is to gather useful data without causing unnecessary anxiety.
When you first begin daily bp tracking or start a new treatment, your doctor may recommend a more intensive schedule. A common approach is to measure your blood pressure twice in the morning before medication and twice in the evening for one full week. This focused period provides a reliable average, giving your doctor a clear and accurate baseline that isn't influenced by the stress of a clinic visit.
Once you and your doctor have a stable plan, this blood pressure monitoring frequency can usually be relaxed. For long-term maintenance, checking your numbers a few times a week is often enough to confirm things are on track. The goal is to stay aware of your body’s patterns, not to obsess over every small fluctuation. This awareness becomes even more powerful when you learn to recognize the surprising daily habits that can spike your numbers.
The Surprising Daily Habits That Can Spike Your Numbers
You already know that a morning run or a strong cup of coffee can move your numbers, but what about the less obvious culprits behind those confusingly high readings? Understanding the common, temporary factors that affect blood pressure readings can help you avoid unnecessary worry. Your body is dynamic, and your blood pressure naturally responds to your environment and actions in ways you might not expect.
Many of these temporary spikes are caused by something called vasoconstriction, which is simply your blood vessels narrowing for a short time. When this happens, your heart has to work harder to push blood through the smaller space, raising your pressure. Some surprising triggers for this include:
- Having a full bladder
- Feeling cold
- Taking certain over-the-counter decongestants
- Being in an emotional or heated conversation
This is precisely why the 'notes' column in your log is so valuable. Jotting down “felt cold” or “took a decongestant” next to a high reading provides crucial context. It helps you and your doctor distinguish between a random spike from one of these temporary high blood pressure causes and a consistent pattern that might need attention.
When to Worry: Taking Action on Your Blood Pressure Readings
A single blood pressure reading can feel like a confusing snapshot taken at the doctor’s office. Now you have the tools to see the whole movie. By understanding what the numbers mean and how to capture them accurately, you’ve transformed a moment of uncertainty into a tool for insight.
Putting this knowledge into practice is straightforward. Here is your four-step plan to get started:
- Get a validated upper-arm monitor.
- Follow the 7-step checklist for every reading.
- Keep a detailed log for at least one week before your next doctor's appointment.
- Share your log with your doctor and create a plan together.
This process of home blood pressure monitoring isn’t about diagnosing high blood pressure on your own. It’s about becoming an expert on your own body. The log you create is the most valuable piece of information you can bring to your next appointment.
You are no longer a passenger; you are a co-pilot in your own healthcare. Use this skill not to worry, but to collaborate. The goal is simple: to have a more productive, data-driven conversation when you talk to your doctor, giving you both the confidence to make the best decisions for your heart, together.
Frequently Asked Questions
Question: What do the two numbers in a blood pressure reading mean, and how do I know which category I'm in?
Short answer: The top number (systolic) is the peak pressure when your heart contracts; the bottom number (diastolic) is the pressure while your heart relaxes between beats. Both matter because they show the full cycle of stress on your arteries. To classify your reading, use these ranges:
- Normal: less than 120/80 mmHg
- Elevated: 120--129 systolic and less than 80 diastolic
- Hypertension Stage 1: 130--139 systolic or 80--89 diastolic
- Hypertension Stage 2: 140 or higher systolic or 90 or higher diastolic
- Hypertensive crisis: higher than 180/120 mmHg (seek immediate care) The "and/or" matters: Elevated requires systolic 120--129 and diastolic under 80. For Stage 1 and Stage 2, either number in range places you in that category. Examples: 135/85 is Stage 1; 125/78 is Elevated; 115/75 is Normal.
Question: If high blood pressure has no symptoms, why should I worry?
Short answer: Hypertension is called the "silent killer" because it quietly damages your arteries and organs over time even when you feel fine. Constant high pressure stiffens and narrows arteries, forcing your heart to work harder and raising risks like heart failure, stroke, and kidney damage. Since you can't rely on symptoms, regular monitoring is the only way to detect problems early and protect your long-term health.
Question: What's the right way to measure my blood pressure at home, and which monitor should I buy?
Short answer: Aim for a true resting measurement and follow a consistent routine:
- Sit quietly for 5 minutes.
- Sit with your back supported, feet flat, and legs uncrossed.
- Rest your bare arm at heart level.
- Take 2--3 readings one minute apart and average them. For most people, a clinically validated upper arm cuff is more accurate and reliable than a wrist monitor because it measures at a larger artery and is less sensitive to arm position. Wrist monitors can misread if your wrist isn't exactly at heart level. A validated upper arm model (for example, from Omron) is a dependable choice.
Question: What diet changes actually lower blood pressure?
Short answer: Start by cutting excess sodium and adding DASH-friendly foods. Sodium makes your body hold onto extra fluid, which raises blood volume and pressure. Most sodium (over 70%) comes from processed and restaurant foods---often "hidden" in items like bread, cereals, canned soups, and salad dressings---so read labels and compare brands. The DASH diet (Dietary Approaches to Stop Hypertension) helps lower blood pressure, often within weeks, by emphasizing foods rich in potassium, calcium, and magnesium. Build meals around fruits and vegetables, whole grains, lean proteins (fish, poultry), low-fat dairy, and nuts, seeds, and beans.
Question: When does a high reading become a medical emergency?
Short answer: A reading of 180/120 mmHg or higher is a hypertensive crisis and requires prompt medical attention. It's a potential emergency---call 911 immediately---if it's accompanied by symptoms such as severe headache, shortness of breath, chest pain, sudden numbness or weakness (especially on one side), vision changes, or trouble speaking. Do not drive yourself; paramedics can begin care right away.
Question: What does “mmHg” mean in a blood pressure reading?
Short answer: It stands for millimeters of mercury, the standard unit used to express pressure. When you see a reading like 120/80 mmHg, both numbers are measured in this unit—it's simply the medical standard for reporting blood pressure.
Question: My reading is in the Elevated range—what should I do next?
Short answer: Elevated (120–129 systolic and less than 80 diastolic) is a yellow-light warning, not yet hypertension. It’s your chance to act early. Start small, consistent changes: measure your blood pressure regularly, cut back on sodium (read labels and compare brands), add DASH-style foods (fruits/vegetables, whole grains, lean proteins, low-fat dairy, nuts/beans), move more (a simple daily walk toward 150 minutes/week), and prioritize stress management and restful sleep. Pick one manageable step this week and build from there.
Question: How can I tell if low blood pressure (hypotension) is a problem for me?
Short answer: Low blood pressure is usually only a concern if it causes symptoms. Warning signs include dizziness or lightheadedness (especially when standing), fainting, blurred vision, nausea, and unusual fatigue. Common temporary triggers include dehydration, certain medications, or standing up too quickly. If these symptoms happen often, mention them to your doctor and track your readings at home to provide helpful context.
Question: How do stress and poor sleep keep my blood pressure high?
Short answer: Stress releases hormones like adrenaline that make your heart beat faster and narrow your blood vessels—pushing your numbers up. When stress is chronic, your body never gets the “all-clear,” so pressure stays elevated. Sleep should naturally lower blood pressure, giving your heart and vessels time to recover. Poor or insufficient sleep robs you of this reset, keeping your cardiovascular system under strain. Prioritizing relaxation and protecting quality sleep are essential parts of blood pressure control.
Question: What’s the connection between high blood pressure and kidney health?
Short answer: Chronically high pressure damages the kidneys’ tiny, delicate blood vessels, reducing their ability to filter waste and excess fluid. Damaged kidneys then struggle to regulate fluid and may release hormones that raise blood pressure further—creating a dangerous two-way cycle. That’s why clinicians monitor both your blood pressure and kidney function, and why controlling blood pressure is key to protecting your kidneys.