Filter
53 products
Type: Nursing
3M Micropore Surgical Tape Box
Type: Nursing
Uro Bag Romo 10 DB-1070-10 (Pack of 10)
Type: Nursing
Gauze Than 90cm x 18mtr (1 than)
Type: Nursing
Mackintosh Sheet Mattress Protector for Bed (10m)
Type: Nursing
JMS Medi Tape Micropore Dressing
Type: Nursing
Nel Cath GS 1004
Type: Nursing
SafeCath Silicon Two Way Foleys Cathete
Type: Nursing
BARD Winged Infusion Set
Type: Gauzes
Sterile Gauze 12 Ply Swab Dressing (100 Pc - 25 packs of 4 Each)
Type: Nursing
Yankur Suction Set Handle with 2Mtr Tubing
Type: Nursing
Karman type Cannula with Adaptor (pack of 25)
Type: Nursing
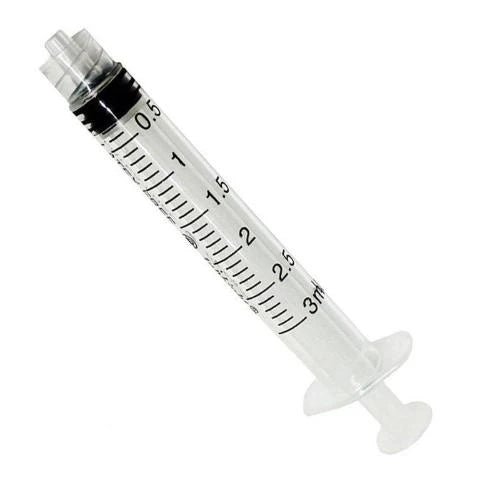
BD Syringe 3ml Luer Lock (Pack of 100)
Type: Nursing
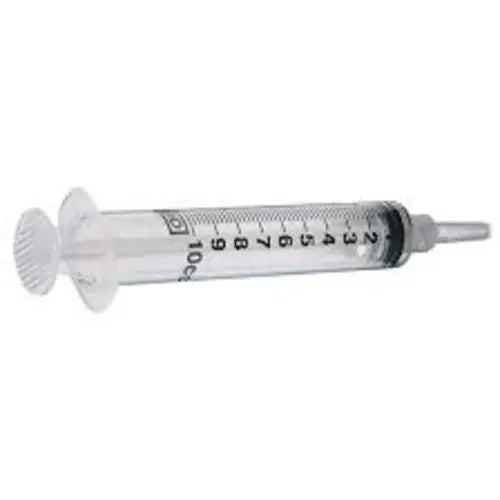
BD Luer-Lock Syringe 10ml (Pack of 100)
Type: Nursing
BD Discardit II Syringe 20ml (Pack of 80)
Type: Nursing
Umblical Cord Clamp Sterile (Pack of 100)
Collection:
Nursing
Essential Nursing Products Every Nurse Needs
You’re sitting in a hospital bed when a nurse enters, carrying a small tray. You recognize the gloves, but your eyes fix on the other items: the little clip that glows red on your finger, the odd-looking syringe without a needle, and the specific type of wipe they use right before a shot. These aren't random gadgets; every single item has a crucial job directly related to your well-being.
That feeling of uncertainty is completely normal. For most of us, unfamiliar medical equipment can be intimidating, sparking questions like, "What is that for?" or "Is that going to hurt?" But what if you knew that the glowing finger clip is simply a painless way to check your oxygen, like a tiny "check engine" light for your breathing? This guide transforms that anxiety into understanding by explaining the purpose behind these essential nursing products.
In practice, a nurse’s toolkit is built around safety and information. From a simple alcohol swab to a beeping monitor, each item is chosen to do one of two things: protect you from harm or give the nurse a clear picture of what’s happening inside your body. We are going to explore what do nurses use and reveal the simple, practical reasons behind their choices, showing how each one contributes to better, safer care.
Consider this your tour of the hospital tools explained in plain English. We’ll start with the basics and work our way up, demystifying the equipment you’re most likely to see. By the end, you’ll see that a nurse's tray isn't filled with scary instruments, but with carefully selected tools designed to keep you comfortable, safe, and on the path to healing.
What a Stethoscope Can Really Hear (And Why It’s Not Just for Heartbeats)
When a nurse places that cool, metal disc on your chest, you probably assume they’re only listening to your heartbeat. That’s certainly one of its jobs, but a stethoscope is a powerful diagnostic tool that reveals secrets from all over the body. It’s an expert listening device, allowing a nurse to hear what’s happening inside your lungs. They’re listening for the clean, quiet sound of air moving freely. If they hear crackling or bubbling, it could be a sign of fluid buildup, like with pneumonia. This simple act of listening helps them understand how well you’re breathing long before it becomes a visible problem.
Beyond the chest, that same stethoscope often travels down to your abdomen. After a surgery or during a stomach illness, a nurse might listen for what are called “bowel sounds.” The gurgles and rumbles we sometimes hear are actually a great sign—they mean your digestive system is awake and moving things along. If it’s too quiet, it might signal a problem. Sometimes a nurse will flip the chestpiece over to the smaller, bell-shaped side; it’s designed to pick up lower-pitched sounds, giving them a more complete picture of what’s going on inside.
You’ve probably also noticed that a nurse doesn’t just listen in one spot. When they move the stethoscope across your back or belly, they are methodically mapping out the area. Each position gives them a sound-snapshot of the organ underneath. By listening to your lungs in six or eight different places, they can pinpoint exactly where a problem might be, rather than just getting a general impression. It’s this careful, detailed listening that turns a simple tool into an essential part of keeping you safe and healthy.
The Secret Behind the Squeeze: What a Blood Pressure Reading Actually Means
Everyone is familiar with the tightening squeeze of a blood pressure cuff around their arm. But what do the two numbers that pop up on the screen actually mean? Think of your arteries as a garden hose. The top number, called systolic pressure, measures the force when your heart beats and pushes blood out—like turning the hose on full blast. The bottom number, or diastolic pressure, is the pressure that remains in the arteries while your heart is resting between beats. Together, these numbers give a nurse a clear picture of the stress on your circulatory system.
You might have noticed a nurse pausing to select a specific cuff for your arm. That choice is critical for getting an accurate reading. Using a cuff that’s too small for your arm can artificially inflate the numbers, making your blood pressure seem higher than it really is. Conversely, a cuff that’s too large can give a falsely low reading. This careful step ensures the information they gather is reliable, forming a trustworthy foundation for any health decisions.
Ultimately, that reading is a vital clue about what’s happening inside your body. High blood pressure suggests your heart is working too hard to pump blood, which can strain your organs over time. Low blood pressure, on the other hand, might mean your vital organs aren’t getting enough oxygen-rich blood to function well. This is why the cuff is one of the most essential nursing products; it provides a quick, non-invasive snapshot of your overall health. It’s a powerful assessment, just like the one a nurse can perform with a simple beam of light.
More Than a Flashlight: How a Tiny Light Checks Your Brain’s Health
That simple beam of light often comes from a tool that looks like a small flashlight: a nurse’s penlight. Its most important job isn’t just to help see in the dark, but to perform a quick, crucial check on your brain function. When a nurse shines the light into your eyes, they’re watching your pupils. A healthy, automatic response is for your pupils to get smaller. This pupillary light reflex is a direct signal that the nerve pathways between your eyes and your brain are working exactly as they should.
You may have also noticed a series of black dots or circles of increasing size on the side of many penlights with a pupil gauge for nurses. This isn’t a decoration; it’s a ruler. A nurse compares your pupil size to these circles to get an exact measurement in millimeters. This step removes guesswork, allowing them to accurately record your status. Documenting that a pupil is "3mm" is far more useful for tracking changes than simply writing "small," ensuring every member of a care team is on the same page.
Ultimately, this two-second test provides an incredible amount of information. If one pupil reacts differently than the other, or if they don't react at all, it can be an early warning sign of a head injury or another serious neurological issue. It’s one of the fastest, non-invasive ways to assess what's happening inside the body. But to keep both themselves and their patients safe on the outside, nurses rely on another fundamental tool for protection.
Beyond Germs: The Two-Way Safety of a Nurse’s Gloves
Of all the essential nursing products, gloves are perhaps the most recognizable. We instinctively understand they form a barrier, protecting the nurse from blood or other bodily fluids. But the safety works both ways. A fresh pair of gloves also protects you, the patient, from any stray germs the nurse might have on their hands, ensuring the care you receive is as clean and safe as possible. This dual protection is fundamental to modern medicine.
This is also why you'll see nurses change gloves so frequently, sometimes even for different tasks with the same patient. Think about it like cooking in your kitchen: you wouldn’t handle raw chicken and then chop a salad with the same unwashed hands. In the same way, a nurse will change gloves after touching a bedrail before they handle a clean dressing. This simple habit prevents germs from one surface from being accidentally carried to another, a critical step in stopping infections before they can start.
So, while it might seem wasteful, each new pair of gloves represents a powerful commitment to safety. This simple, disposable item is one of the most effective tools for preventing the spread of illness within a hospital. This dedication to a germ-free environment also explains why an alcohol wipe isn't just for a "quick clean."
Why an Alcohol Wipe Isn't Just for a "Quick Clean"
We’ve all felt that cold, quick swipe of an alcohol pad right before a shot or a blood draw. It’s easy to think of it as just wiping away a bit of surface dust, but its job is far more critical. This is where we see the difference between simple cleaning and medical disinfecting. While cleaning might remove visible dirt, disinfecting actually kills the microscopic germs—the bacteria and viruses—that you can’t see. That little wipe is a powerful tool designed specifically to create a safe, germ-free zone on your skin.
Have you ever noticed how a nurse will pause for a moment after wiping your skin? That brief wait is the most important part of the process. For the alcohol to effectively kill the germs, it needs time to evaporate and air dry completely. It’s during this evaporation that the alcohol breaks down the bacteria. Blowing on the area to speed it up or wiping it with a piece of gauze actually makes it less effective. That small moment of stillness is what ensures the job gets done right.
This simple, ten-second routine prevents a significant risk. Your skin is naturally home to plenty of bacteria that are harmless on the surface. However, if a needle were to push those same bacteria underneath your skin and into your tissue or bloodstream, they could cause a painful and serious infection. The alcohol wipe is a fundamental safety tool that stops this from happening. This careful attention to protecting the skin is also why, when it comes to covering a wound, the choice between using gauze versus a simple cotton ball is so deliberate.
Gauze vs. Cotton Balls: Why What Covers a Wound Matters
After protecting the skin before a needle, a nurse’s next focus is often protecting it after an injury. You might be tempted to grab a soft cotton ball for a cut, but a nurse will almost always reach for a woven gauze pad. Why? Cotton balls are made of loose fibers that can easily pull apart and get stuck inside a wound. These tiny threads act like splinters, preventing the skin from closing and potentially trapping bacteria, which can lead to a nasty infection and slower healing. Gauze, on the other hand, is designed to be strong and lint-free, so it absorbs fluid without falling apart.
Securing that gauze brings up another common question: isn't tape just tape? Not in a medical setting. Nurses have a whole toolkit of different tapes because skin isn't one-size-fits-all. For fragile or elderly skin, they might use a gentle paper tape that peels off without causing damage. For a bandage over a joint like an elbow or knee, a flexible cloth tape that stretches with your movement is a better choice. The goal is always to hold the dressing securely while being as kind to the surrounding skin as possible.
Ultimately, the combination of the right dressing and tape creates an ideal healing environment. A proper bandage does two critical jobs: it acts as a physical barrier to keep out dirt and germs, and it absorbs any drainage from the wound, keeping the area clean. By creating this protected, clean space, the dressing allows your body’s natural healing processes to work efficiently, which often means healing faster and with less scarring.
This careful attention to what's happening on the surface of the body is matched by an equal focus on monitoring what’s happening inside. Just as the right dressing helps a wound heal, simple devices can give a nurse a quick snapshot of your internal health. One of the most common is that little glowing finger clip.
The Glowing Finger Clip: How a Pulse Oximeter Instantly Checks Your Breathing
That small device a nurse clips onto your finger is called a pulse oximeter. It shines a harmless red light through your skin to get a quick and painless reading of two vital signs: your heart rate and, more importantly, the oxygen level in your blood. Think of it as an instant “check engine” light for your body's oxygen supply. It’s one of the most essential nursing products because it provides critical information in just a few seconds, without needing a needle or any complex setup.
When you look at the oximeter’s screen, you’ll see a percentage, often between 95% and 100%. This number represents your oxygen saturation—in other words, how much of your blood is currently full of the oxygen you’ve just breathed in. A number in that high range tells a nurse that your lungs are doing a great job of capturing oxygen and your heart is effectively pumping it to the rest of your body, which is crucial for everything from thinking clearly to healing properly.
The real value of this tool is its power as an early warning system. A drop in oxygen levels can be the very first sign that a patient is developing a breathing problem, sometimes even before they feel short of breath. By monitoring this number, nurses can intervene quickly—perhaps by helping the patient sit up or adjusting their position—to prevent a small issue from becoming a serious one. Just as these monitoring tools are chosen for patient safety, a nurse’s daily uniform is also packed with purpose.
A Nurse’s Uniform: Why Scrubs and Shoes Are Also Safety Equipment
When you picture a nurse, you probably see them in a set of scrubs. But that familiar uniform is much more than a simple dress code; it’s a frontline tool in the battle against infection. Unlike your everyday clothes, scrubs are designed to be washed in extremely hot water with harsh detergents. This industrial-strength cleaning process is powerful enough to kill dangerous germs that can be picked up in a hospital, preventing them from spreading between patients. By wearing durable, medical-grade scrubs that can withstand this daily sanitization, nurses create a safer environment for everyone.
Equally important, though less obvious, is what nurses wear on their feet. A nurse can spend the entirety of a 12-hour shift walking, standing, and rushing from room to room. This constant activity leads to physical exhaustion, and a tired nurse is more likely to make a small error. Because patient safety is the absolute priority, finding the best shoes for nurses on their feet all day is not about comfort alone—it’s about ensuring they stay sharp and focused. This is often why you’ll see them wearing specific clogs or sneakers, sometimes paired with comfortable compression socks for 12-hour shifts, to fight fatigue.
These specialized shoes are another form of Personal Protective Equipment (PPE), chosen for specific safety features you won’t find on a typical sneaker. The most critical features include:
- Non-slip soles to prevent falls on freshly cleaned or unexpectedly wet floors.
- A closed-toe design that protects their feet from dropped sharp objects or hazardous fluid spills.
- Exceptional cushioned support to absorb shock and reduce the muscle strain that leads to fatigue.
From their germ-resistant scrubs to their fatigue-reducing footwear, every part of a nurse's attire is a deliberate choice aimed at protecting both themselves and their patients. But what about the smaller, essential items they keep within arm's reach? That’s where you’ll find a universe of tools designed for faster, more effective care.
A Universe in Their Pockets: The Tools a Nurse Carries for Faster Care
If you've ever wondered what do nurses carry in their pockets, the answer is a mini-arsenal of tools for immediate action. Many use a pocket organizer for nursing scrubs to keep everything in its place, because in an urgent situation, fumbling for a tool wastes precious seconds. This is a core part of knowing how to pack a nursing clinical bag or pocket for a shift. A quick look inside would often reveal items like:
- Trauma Shears/Scissors
- A roll of medical tape
- Saline flushes
- Multiple pens (black, blue, red)
- A penlight
- Alcohol wipes
While some of those items are familiar, others have a very specific job. Take trauma shears, for example. These aren't your average office scissors. They are built with a blunt, angled tip and are powerful enough to cut through tough materials like denim, seatbelts, or even a penny, all without accidentally poking or cutting the patient's skin. In an emergency where clothing needs to be removed in a hurry to access an injury, these specialized shears are indispensable for providing fast, safe care.
The "Highway" into Your Body: Understanding IV Lines and Pumps
Few pieces of hospital equipment are as common as the IV line. That thin, flexible tube is technically called an intravenous catheter—"intra" (inside) and "venous" (vein)—and it creates a direct highway into the body. For situations where medicine or fluids are needed quickly, this route is far more effective than waiting for a pill to make its way through the digestive system. An IV line allows nurses to deliver hydration, nutrition, or critical medication straight into the bloodstream for immediate effect, making it one of the most essential nursing products for patient care.
To make sure this highway stays open and clear, nurses perform a simple but vital safety check using a saline flush. Before giving medication, you’ll see them attach a small syringe filled with sterile salt water and gently push it into a port on the IV tubing. Think of it like running clean water through a tiny pipe to ensure it’s not clogged. This quick step confirms the line is working properly, so you can receive your treatment safely and effectively. It’s a small action that plays a huge role in patient safety.
Often connected to the IV is a machine that beeps—the IV pump. While the sounds can sometimes feel alarming, this device is your personal safety regulator. It acts like a cruise control for medicine, precisely managing the speed and amount of fluid you receive down to the milliliter. This technology ensures you get exactly the right dose over the correct amount of time. The beeps simply alert the nurse when the medication bag is empty or if the line needs checking, turning a potentially intimidating noise into a sign of vigilant, personalized care.
From Mystery to Meaning: How Understanding Your Care Empowers You
A tray of medical supplies might have once seemed intimidating—a collection of unfamiliar objects and strange-sounding names. Now, you can see beyond the plastic and steel. You know that a stethoscope is for listening, that gauze is for protecting, and that each item has a specific job rooted in care and compassion.
From the simple observation of a blood pressure cuff to the life-sustaining delivery of an IV line, you’ve journeyed through a nurse's toolkit. You now understand the core principle that unites every product: patient safety. Each tool, whether a humble pair of gloves or a complex monitoring device, is an extension of a nurse's hands, eyes, and ears, all working together to help the body heal.
This new knowledge is more than just trivia; it's a tool for you. The next time you find yourself in a medical setting, try this: when you see a piece of equipment, ask yourself, "What is this helping the nurse to do for me?" This simple question, backed by your understanding of medical supplies, shifts your perspective from a passive patient to an informed participant. This is the foundation of patient education.
That shift is where your power lies. You will no longer see just a tray of confusing equipment; you will see tools for listening, for protecting, and for healing. This understanding has the power to transform anxiety into confidence, allowing you to ask better questions and become an active, engaged partner in your own health journey.