Filter
5 products
Type: General
Taylor Neurological Knee Hammer
Type: General Accessories
Neurological Knee Hammer Set
Type: Accessories
Percussion Chrome Plated Handle Knee Hammer Taylor Model
Type: General Accessories
Goniometer Set for Joint Angle Measurement Tools
Type: Clinical Assessment
T Shaped Hammer for Clinical Use
Collection:
How to Use a Knee Reflex Hammer
You're sitting on the edge of an exam table, the paper crinkling beneath you. The doctor pulls out that little rubber hammer, and you know what's coming next. But have you ever wondered why your leg kicks out all by itself? It's not a party trick; it's a high-speed data check on your body's wiring, providing a nearly instant snapshot of your health.
So, why do doctors tap your knee? The answer has less to do with your joint and more to do with the vast communication highway running through your body: the nervous system. The familiar knee-jerk reflex is one of the quickest ways for a physician to check if that system is running smoothly. In practice, the test is a clear window, revealing how well messages are traveling between your spinal cord and muscles---all without your brain even getting involved.
This article breaks down exactly what happens during that split-second kick and what a doctor is looking for in your response. You'll understand the elegant shortcut your body takes and see why the humble medical reflex hammer remains an essential tool, offering powerful insights with just one simple, well-aimed tap.
What Exactly Is a Reflex Hammer? More Than Just a Little Mallet
That little mallet your doctor pulls out might look simple, but it's a finely tuned diagnostic instrument. A reflex hammer is used for one primary job: to safely and reliably test your body's reflexes. Unlike a tool for construction, its purpose isn't to drive a nail, but to deliver a very specific tap that provides a quick window into the health of your nervous system. It's one of the most classic and efficient tests in medicine.
The most important feature is the soft rubber head. This design allows a doctor to firmly tap a specific target---a tendon---without causing pain or injury. Think of a tendon as the tough, rubber-band-like cord connecting a muscle to a bone. The hammer's job is to momentarily stretch this tendon, much like gently plucking a guitar string, to see how the body's "wiring" responds.
By delivering this quick, focused stretch, the medical reflex hammer starts a chain reaction that happens faster than you can think. This simple action is the key that unlocks the reflex. This reaction is all about a clever shortcut your body uses every day.
The "Magic" Explained: How Your Leg Kicks Before Your Brain Knows
That automatic kick isn't a party trick; it's a clever biological shortcut called a spinal reflex. Think of your nervous system as a corporate office. For most actions, like deciding to walk across a room, a request goes all the way up to the "CEO"---your brain---for a decision. A reflex, however, is more like pulling a fire alarm. The signal doesn't need to travel all the way to the top. Instead, it goes to a local manager---your spinal cord---which has standing orders to react immediately, no questions asked.
This simple and lightning-fast pathway is called a reflex arc. The patellar reflex test can be broken down into four key steps:
- The Tap: The reflex hammer gently but quickly stretches the patellar tendon below your kneecap.
- The Message Up: A sensory nerve in the tendon instantly sends an "Alert!" signal straight to your spinal cord.
- The Spinal Cord Shortcut: Bypassing your brain completely, the spinal cord immediately sends a "Contract!" command back down a different nerve.
- The Kick Back: This command reaches the large muscle in your thigh (the quadriceps), causing it to tighten and kick your lower leg forward.
Because your brain is left out of this initial loop, you can't consciously stop the kick from happening. That's the whole point. This involuntary nature is precisely what makes eliciting the patellar reflex such a reliable diagnostic tool. It shows the doctor how your body's basic wiring is functioning without any interference from your conscious thoughts.
By observing the speed and strength of the kick, a doctor gets an instant status report on the health of your nervous system. It's a remarkably effective way to perform a quick assessment of the nerve pathways that connect to your lower spine. Of course, triggering this response depends entirely on a doctor's ability to tap the exact right location.
Where to Tap: Finding the Sweet Spot for the Patellar Reflex
Triggering that reflex arc isn't a matter of luck; it's a matter of location. The doctor isn't just randomly tapping your knee area. They are aiming for a very specific target known as the patellar tendon, the tough, flexible band that connects your kneecap (the patella) to your shinbone. Hitting this exact spot is the key to creating the quick stretch that kicks off the entire reflex message.
You can actually find this "sweet spot" on your own knee quite easily. Sit down and let your leg relax and hang freely, so your knee is bent at about a 90-degree angle. Now, feel for the hard, round bone of your kneecap. Just below it, before you get to the hard ridge of your shinbone, you'll find a softer, slightly recessed area. As shown in the photo, this is the patellar tendon. If you press gently, it feels less like bone and more like a thick, firm rubber band under the skin.
This small band of tissue is so important because it's packed with the special sensors that detect stretching. When the reflex hammer taps it, these sensors are what send that urgent signal to your spinal cord. Tapping the hard kneecap itself or the large thigh muscle won't work, because it bypasses this specific alarm system. Think of it like pressing a doorbell button versus knocking on the wall next to it---only the button is wired to make the chime ring. This need for precision is exactly why your doctor still relies on this seemingly simple test today.
Why Your Doctor Still Uses This "Old-Fashioned" Test Today
So why is it still a staple in every doctor's toolkit? The answer is efficiency. That quick knee-jerk reaction provides an immediate and surprisingly informative status update on your body's wiring, all without the need for expensive or time-consuming equipment. Its physiological significance lies in its ability to perform a rapid "signal check" on a specific nerve pathway, making it one of the most effective frontline screening tools in medicine.
At its core, the test is a way to see how well messages are traveling between your spinal cord and your muscles. Think of it like checking your home's Wi-Fi signal. A quick, crisp kick is like having a strong, full-bar connection---it suggests the signal from your spinal cord is reaching your leg muscle without interference. If the reflex is weak, absent, or even unusually strong, it's like a buffering video or a dropped signal. It tells the doctor there might be an issue somewhere along that communication line that's worth a closer look.
The result is a clue, not a conclusion. An abnormal reflex doesn't instantly mean something is wrong; it simply gives your doctor a valuable piece of information. Like a detective finding a single footprint at a scene, what the test indicates is simply a starting point that helps a professional know where to focus their investigation. It's this power---to reveal so much, so quickly---that ensures the humble neurology hammer remains an essential diagnostic tool.
What a "Normal" Reflex Looks and Feels Like
It's natural to wonder if your leg kicked out "enough" during a reflex test, but there's no gold medal for the strongest kick. The reality is that the range of normal responses is incredibly wide. Some people have a barely-there flicker of movement, while others have a surprisingly brisk kick. Neither is inherently better. A doctor is less concerned with the raw strength and more interested in what is normal for you. Think of it like handwriting---everyone's is a little different, but as long as it's consistent and legible, it's considered normal. The goal isn't to score high on a deep tendon reflex grading scale, but to show a clear and consistent response.
Sometimes, a reflex can be shy. If you're nervous, cold, or even just thinking too hard about not kicking, your reflex might seem absent. When this happens, a doctor may use a simple trick for eliciting the patellar reflex known as the Jendrassik maneuver technique. They'll ask you to hook your fingers together and pull your hands apart with all your might, right as they tap your knee. This action of straining your upper body acts as a clever distraction for your nervous system. It overrides your conscious tension, allowing the pure, automatic reflex in your leg to show itself without interference.
Ultimately, what matters most to your doctor is consistency and symmetry. A reflex that is present---even if it's on the weaker side---is usually a good sign, especially if the reflex in your other knee is about the same. It's a sudden change in your typical reflex, or a major difference between your left and right sides, that provides a useful clue. This comparison is the first step in determining whether a reflex is simply your personal "normal" or if it might be something more.
When Kicks Are Weak or Strong: What an Abnormal Reflex Can Mean
While a consistent kick on both sides is the expected outcome, sometimes the response is different. A weak or absent reflex can act as a clue that the nerve "circuit" is being interrupted somewhere. Think of it like a faint radio signal; the problem could be with the transmitter (the nerve sending the signal), the receiver (the muscle), or anywhere along the pathway. This tells a doctor that the communication line for that specific part of the body might need a closer look, which helps them narrow down their investigation.
Conversely, a reflex can sometimes be much stronger than expected, causing the leg to jump with surprising force. This type of exaggerated response can suggest a different kind of issue. If a weak reflex is like a poor signal, an overly strong one is like having the volume control turned all the way up without a way to moderate it. It often suggests that the central nervous system---the brain and spinal cord, which normally help keep reflexes in check---isn't providing its usual calming influence, causing the local reflex to overreact.
A reflex finding is not a diagnosis, but a single data point that a doctor interprets within the context of your entire physical exam. An abnormal reflex in one knee tells a very different story than one that appears in both legs and both arms. The specific location and type of change are what transform a simple kick into a valuable piece of the diagnostic puzzle, guiding the next steps of a medical evaluation.
For this reason, you should never try to interpret your own reflexes. Many factors, from stress to the temperature of the room, can influence the result, and there are many potential causes for an abnormal deep tendon reflex. Only a trained professional can distinguish between a temporary quirk and a meaningful clinical sign. To gather these clues effectively, doctors use more than just a tap on the knee, employing a whole toolkit of techniques and instruments to get a complete picture.
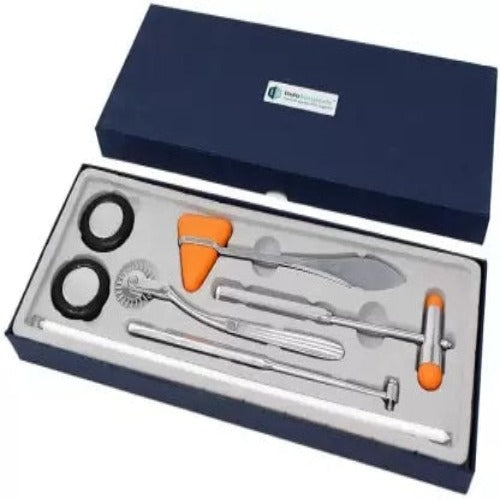
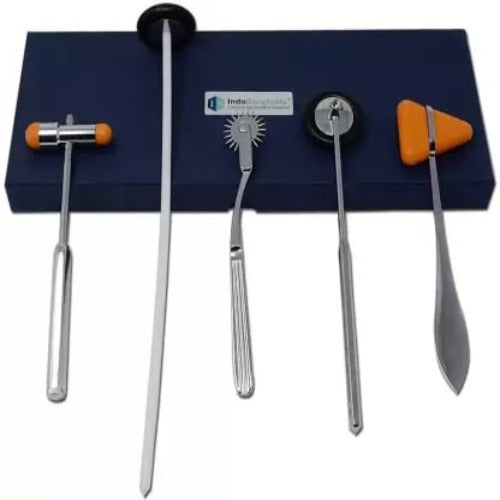
A Tour of the Toolkit: Why There Are So Many Types of Reflex Hammers
While the little triangular "tomahawk" hammer is the most recognizable, you might be surprised to learn it's just one of several types of neurological hammers in a doctor's toolkit. Just as a mechanic needs more than one kind of wrench, a doctor may choose a specific hammer to get the clearest possible picture of your nervous system's health. The design isn't for looks; it's all about function.
The most common tool is the Taylor hammer, with its classic triangular rubber head and flat metal handle. It's lightweight, durable, and easily fits into a lab coat pocket, making it perfect for routine physicals and quick screenings. Its design requires a quick, deliberate flick of the wrist to work effectively, something most general practitioners have mastered. It's the reliable workhorse of the reflex hammer world.
For more detailed neurological exams, specialists often prefer different designs. The Babinski hammer, for example, features a round, metal-rimmed head on a handle that often unscrews or telescopes for portability. Its heavier head allows the doctor to use a more passive, pendulum-like swing, letting the weight of the hammer do the work. This can produce a more consistent tap, which is useful when comparing subtle differences between reflexes.
Another specialist favorite is the Queen Square hammer. With its long, flexible handle and a soft plastic disc for a head, it looks quite different from the others. This design is all about momentum. The long handle allows for a large, slow swing that is very gentle on the patient but highly effective at triggering a reflex, making it ideal for situations where reflexes are difficult to elicit. The choice between these reflex hammer types ultimately comes down to the doctor's training, personal preference, and the specific information they need to gather.
Not Just for Knees: Other Places Doctors Check Your Reflexes
While the knee-jerk reaction is the most famous, it's just the opening act of a much broader performance. That simple leg kick gives a doctor a snapshot of one specific nerve pathway. But to get a more complete picture of your nervous system's health, they often need to check a few other key locations, turning a single test into a quick, full-body tour.
Think of your nervous system as the electrical wiring of a house; you wouldn't just test one outlet to see if everything is working. Similarly, a doctor might test reflexes in several spots. You'll likely notice them tapping:
- The back of the ankle (Achilles reflex): Causing your foot to point down.
- The inside of the elbow (Biceps reflex): Making your forearm twitch or flex.
- The back of the upper arm (Triceps reflex): Prompting your arm to straighten.
Each of these tests checks a different set of "circuits" connecting your muscles to your spinal cord. By comparing the responses---whether they are strong, weak, or absent---from different parts of your body, a doctor can more effectively pinpoint where a potential issue might be located. A consistent pattern of responses across all these points is just as informative as the result of a single tap, providing a richer, more detailed story about your body's wiring.
The Pointy End and the Brush: What Are the Other Gadgets For?
If you've ever looked closely at a reflex hammer, you might have noticed it's more than just a mallet. Many models, like the popular Taylor or Babinski hammers, have a pointed plastic tip at the end of the handle. This isn't for delivering a sharp poke; it's a key part of a sensory test. With your eyes closed, a doctor might lightly touch your skin with either the soft rubber head or the pointed tip, asking you to distinguish between "dull" and "sharp." Some hammers even have a small brush that unscrews from the handle, used to test your perception of light touch.
This shift from tapping a tendon to touching the skin is a clever diagnostic move. While the reflex test checks the high-speed "shortcut" circuit in your spinal cord, this sharp/dull discrimination test examines a different pathway entirely: the one that sends sensation messages from your skin all the way up to your brain. Think of it this way: the reflex tap tests if your body's "automatic alarm" works, while the sensory test checks if your brain is getting the "manual report" clearly.
For an even more detailed map of sensation, a doctor might use another one of the classic neurological examination instruments: the Wartenberg wheel. This device looks like a small pinwheel with sharp, but not skin-piercing, points. By gently rolling it across your arms, legs, or torso, a clinician can perform a more precise sensory test, identifying if there are specific areas where the sensation feels dull, different, or absent. These simple tools, often found on or alongside a standard neurology hammer, help build a complete picture of your nervous system's communication network.
The Simple Hammer's Lasting Power in a High-Tech World
That familiar tap-and-kick routine is no longer a mystery. Where you once saw a curious medical ritual, you can now see the elegant, high-speed conversation happening inside your body. You understand that the kick isn't a choice but a brilliant shortcut---a signal that travels from a tendon to your spinal cord and back to a muscle in the blink of an eye, completely bypassing your conscious thought.
This is the simple power of the medical reflex hammer. That one tap gives a doctor a remarkably quick status report on your nervous system's communication lines. Far from being just a tool for the knee-jerk reflex, it's a fundamental diagnostic instrument that turns a simple physical reaction into a valuable clue about your body's hidden wiring.
So the next time you're sitting on that crinkly paper and see the knee reflex hammer come out, you won't just wonder what's happening. You'll understand the elegant, lightning-fast conversation occurring inside your own body---a small tap that tells a big story.
Q&A
Question: What is the knee-jerk reflex actually testing, and why doesn’t the brain get involved?
Short answer: It checks the integrity of a fast, automatic spinal circuit—the patellar reflex arc—linking tendon stretch sensors to the spinal cord and back to the quadriceps muscle. Because this pathway bypasses the brain for speed, the response is involuntary; the strength and briskness of the kick give a quick snapshot of how well signals travel along that lower-spine pathway.
Question: Where exactly should the hammer strike, and how should the leg be positioned?
Short answer: Sit with your leg relaxed and dangling at about a 90-degree knee angle. Find the kneecap, then tap the softer, springy band just below it—the patellar tendon—above the hard ridge of the shinbone; avoid tapping the kneecap or thigh muscle. The rubber head provides a quick stretch without causing pain.
Question: What if my leg doesn’t kick at all?
Short answer: It’s often due to tension, cold, anticipation, or simply missing the tendon. A clinician may use the Jendrassik maneuver—have you hook your fingers and pull as they tap—to distract you and reveal the reflex, and they’ll ensure a crisp, accurate strike. Even a small flick can be normal; clinicians focus on consistency and side-to-side symmetry.
Question: How should I interpret a weak, absent, or very strong reflex?
Short answer: Treat it as a clue, not a conclusion. Weak or absent responses can indicate a disrupted circuit anywhere from sensory nerve to muscle; overly brisk reflexes can suggest reduced “calming” control from the brain or spinal cord. Doctors compare both sides and test multiple reflexes before deciding what, if any, further evaluation is needed—self-interpretation can be misleading.
Question: Do different reflex hammers matter, and what else can they test besides the knee?
Short answer: Yes—designs serve different exam styles: the Taylor (tomahawk) is light and wrist-flicked, the Babinski has a heavier, pendular head, and the Queen Square uses a long, flexible handle for gentle momentum. Many include a pointed tip and brush for sharp/dull and light-touch sensory checks, and clinicians also test Achilles, biceps, and triceps reflexes to survey other nerve pathways.