Filter
7 products
Type: Devices
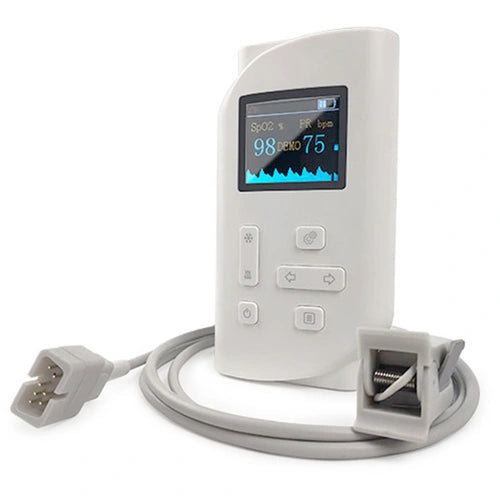
Handheld Pulse Oximeter
Type: Devices
Beurer Pulse Oximeter PO-30
Type: MeddeyGo
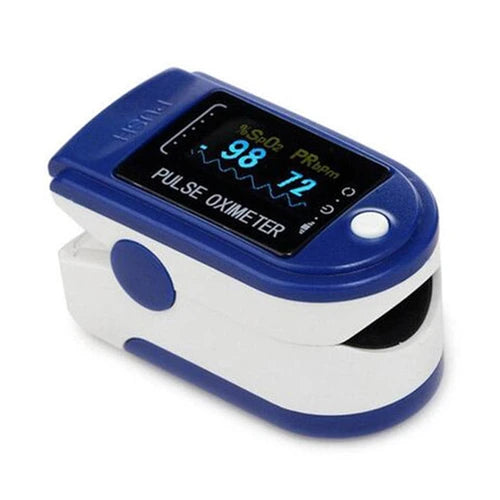
Digital Fingertip Pulse Oximeter
Type: Home Healthcare
Contec CMS50D OLED Fingertip Pulse Oximeter
Type: MeddeyGo
Handheld Pulse Oximeter Delux with Rechargable Battery
Type: pulse oximeter
Contec CMS-60C Handheld Pulse Oximeter
Type: Diagnostic Equipment
Neonatal Pulse Oximeter P Ultra
Collection:
Benefits of Using a Pulse Oximeter
You've likely seen that little glowing red clip at a doctor's office, or perhaps you have one tucked away in your medicine cabinet. This small device, known as a pulse oximeter, has transformed from distinct hospital equipment into a household essential. While purchasing one is simple, understanding exactly what those flashing numbers mean for your personal health requires context.
If you have ever asked yourself what a pulse oximeter tracks, the answer lies in SpO2, or Oxygen Saturation. Imagine your red blood cells are delivery trucks traveling through your body's highways. A blood oxygen monitor checks if they are fully loaded with the "cargo" your organs need to function. SpO2 is the percentage that tells you how full those trucks are, giving you a clear picture of how well your body is fueled.
Confusion often arises when users mix up this oxygen reading with their pulse rate. While your heart rate tells you how fast the engine is running, the oxygen level reveals the quality of the fuel being delivered. You might have a normal heart rate while recovering from a walk, but if your oxygen saturation drops, your body isn't getting the energy it needs. Distinguishing between these two metrics is the first step in effectively using this tool for home wellness.
A reading between 95 and 100 percent is generally considered normal for healthy adults. Seeing a number in this range provides reassurance that your lungs are effectively transferring oxygen into your bloodstream. However, these readings can fluctuate based on posture or activity level, making it crucial to distinguish a genuine health trend from a momentary dip caused by external factors.
Integrating this device into your routine offers a proactive way to listen to your body before you feel physical symptoms. By interpreting your data correctly---and avoiding common pitfalls like cold hands that can skew results---you gain control over your well-being.
The Science of Light: How Infrared Technology Sees Through Your Skin
It seems magical that a small clip can analyze your bloodstream without breaking the skin. The secret lies in physics: light acts differently when it passes through different substances. When you insert your finger into the device, you place your hand between a light source and a sensitive detector. This non-invasive approach allows the oximeter to "look" inside your veins using harmless beams.
Inside the clip, two tiny LEDs shine through your fingernail and tissue. One emits visible red light, while the other sends out invisible infrared light. Blood interacts with them uniquely depending on its oxygen content. Oxygen-rich hemoglobin absorbs more infrared light and lets red light pass through, while oxygen-poor blood does the opposite. The sensor measures how much light passes through your finger versus how much was blocked.
The device essentially analyzes the "color" of your blood. Just as a blushing cheek looks different from a pale one, your blood changes shade based on oxygen levels---bright red indicates high oxygen, while a darker red suggests lower levels. By rapidly comparing the ratio of light absorption, the device calculates your oxygen percentage.
The Delivery Truck Analogy: What Oxygen Saturation Actually Means
When you see a percentage on the screen, the device is grading the efficiency of your blood's transport system. This system relies on hemoglobin, the protein inside red blood cells that acts as the carrier. Like a sponge holding water, hemoglobin grabs oxygen molecules in your lungs and holds them tight as they travel to your brain and muscles. The SpO₂ reading reports how much oxygen your hemoglobin holds compared to its maximum capacity.
To visualize this, imagine your bloodstream is a highway filled with thousands of delivery trucks (red blood cells). If every truck is carrying a full load of crates (oxygen), your fleet is operating at 100% capacity. If some trucks are empty because they couldn't pick up cargo in the lungs, efficiency drops, and less fuel reaches your organs.
A reading of 98% means that for every 100 trucks passing the sensor, 98 are successfully carrying cargo. This resulting number is your blood oxygen saturation level. While 100% is efficient, it is normal for a few trucks to be empty, which is why healthy readings often sit slightly below the maximum.
Decoding the Display: Understanding SpO2, Pulse Rate, and PI Numbers
Device screens often light up with a mix of digits. The largest number, usually labeled SpO₂ , is the percentage of "filled trucks." Sitting next to it is a second value labeled PR or BPM (Pulse Rate). Identifying these labels prevents the mistake of confusing heart speed with oxygen level.
- PR (Pulse Rate): Measured in beats per minute, this tells you how fast your engine is running. A racing heart can sometimes be a response to low oxygen---a frantic dispatcher speeding up deliveries to compensate for empty trucks. A number like 72 means your heart pumps 72 times a minute, distinct from the oxygen reading.
- PI (Perfusion Index): Found on advanced models, this measures pulse strength at the finger. Think of this as signal bars on a cell phone; a low PI indicates weak blood flow (perhaps due to cold hands), making it hard for the monitor to calculate data. A PI above 0.2 usually suggests the sensor has a clear view of your blood flow.
Safe Zones: Differentiating Normal Levels from Emergency Warnings
For most adults, normal blood oxygen saturation levels fall between 95% and 100%. You do not need a perfect 100 to be healthy; a reading of 96% or 97% indicates excellent oxygen transfer. However, personal baselines vary. If you have a chronic lung condition like COPD, your doctor might establish a lower acceptable range, such as 88% to 92%.
Because factors like movement can affect accuracy, always warm your fingers and sit still for a retest if a number looks odd. Use these general guidelines:
- 95%--100% (Normal): No action needed; supply is sufficient.
- 91%--94% (Mild Hypoxia): Evaluate how you feel. If sick, short of breath, or uncomfortable, contact your healthcare provider.
- 90% or Below (Emergency): This typically indicates significantly low oxygen. Seek immediate medical attention.
Relying on a home pulse oximeter gives you clarity to advocate for your health when it matters most.
Choosing the Right Fit: Fingertip vs. Handheld vs. Tabletop Models
Navigating the various types of pulse oximeters begins by looking at your daily routine.
Fingertip Pulse Oximeters offer the balance of portability and simplicity for most home users. These all-in-one clips are wireless and battery-operated, ideal for spot-checking levels before a workout or during the flu. They take a snapshot of your health in seconds and fit easily into a medicine cabinet.
Handheld Pulse Oximeters feature a separate sensor probe connected by a cable to a digital screen. This design allows for easier reading and better sensor stability, often necessary for caregivers monitoring patients who cannot keep their hands steady.
Tabletop / ICU Pulse Oximeters are designed for continuous monitoring. They plug into the wall to track saturation while you sleep or recover, ensuring that a drop in levels triggers an immediate alarm.
Protecting Little Lungs: Why Pediatric Pulse Oximeters Are Unique
Clipping a standard oximeter onto a sick child often results in erratic numbers or a blank screen. This usually isn't a medical emergency, but a mechanical mismatch. If a child's finger is too small, it floats inside the clip, allowing ambient light to flood the sensor or preventing the light beam from aligning with the detector.
Pediatric pulse oximeters are engineered for fingers between 0.3 and 1.0 inches thick. They feature smaller housing for a light-blocking fit and software calibrated for the naturally higher heart rates of children. Many child-specific models include movement-resistant algorithms to distinguish between a squirming hand and the actual pulse beat, preventing false alarms.
The 5-Step Checklist for a Medically Accurate Home Reading
Even high-end gear can be thrown off by environmental factors. Before you clip a device onto your finger, your body needs to be in a steady state. Rushing around raises your heart rate and changes blood flow, skewing data. Follow this protocol:
- Rest: Sit quietly for at least five minutes to return your heart rate to normal.
- Warm Up: Rub your hands together; cold fingers constrict blood flow and hide your pulse.
- Position: Place your hand flat on a table at heart level to reduce gravity's impact.
- Stillness: Clip the device on your middle or index finger and remain still.
- Wait: Ignore initial numbers; wait 30 seconds for the reading to stabilize.
The machine needs moments to lock onto a rhythmic pulse signal. The first number is often a "searching" guess. Once the number stops fluctuating, you have your accurate reading.
Why Nail Polish and Cold Hands Cause False Alarms
Your device relies on light passing through your fingernail, so adding a coat of paint creates a physical barrier. Darker shades like blue, black, or green absorb the red and infrared light the sensor needs, potentially showing a dangerously low reading when you are healthy. While clear or light pink polish might let enough signal through, the safest bet is to use a bare finger or rotate the clip sideways.
Temperature is equally deceptive. When you are cold, your body preserves heat by shrinking blood vessels in your hands (vasoconstriction). This reduces blood volume in extremities, leaving the oximeter with a weak signal. If your hands feel like ice, the sensor might display an error simply because the "traffic" of blood cells is too faint to detect.
Bright room lights or direct sunshine can also overwhelm the internal sensor. Eliminate these external noise factors before assuming your health is in decline.
Spotting Silent Hypoxia: How Your Oximeter Reveals Hidden Dangers
We assume running out of air feels like gasping, but the body can hide distress. "Silent hypoxia" is a condition where saturation levels dip below safe thresholds while you are breathing normally. Your brain generally signals shortness of breath only when carbon dioxide levels rise, not necessarily when oxygen falls. If a virus prevents oxygen absorption without trapping carbon dioxide, your internal alarm system stays quiet.
A reliable blood oxygen monitor bypasses this biological blind spot. It serves as a "check-engine light" for your lungs, revealing a declining fuel supply before your body realizes it is running on empty. Catching these drops early allows for treatment before physical symptoms---like bluish lips or confusion---appear.
Living with COPD: Using SpO2 Monitors for Daily Stability
For those managing chronic conditions like COPD, the standard rules shift. While a healthy adult expects readings above 95%, a doctor might establish a personal target range (often 88%--92%) to prevent over-oxygenation. Monitoring becomes less about spotting emergencies and more about learning your unique baseline.
An oximeter acts as a speedometer for your lungs, helping you pace yourself during exertion or adjust supplemental oxygen. Consistency is key. Maintaining a daily log helps spot trends before flare-ups:
- Time: Time of day.
- Reading: SpO2 % and Pulse Rate.
- Activity: Resting or active?
- Symptoms: Breathless or fine?
Signal Strength Matters: Decoding the Perfusion Index (PI)
The Perfusion Index (PI) is a reliability score for your current measurement. If the PI is low (below 0.4%), the sensor is struggling to detect consistent blood flow. This often happens because hands are cold or the device is positioned incorrectly. Warming your hands or switching fingers can often boost signal strength, turning a confusing error message into a steady result.
You can use this metric to identify which finger provides the strongest connection. You might find your middle finger consistently offers a higher index than your index finger, making it the superior choice for daily checks.
Beyond Oxygen: Why Pulse Rate Detection is a Vital Health Metric
While eyes naturally gravitate toward the SpO₂ percentage, the Pulse Rate (PR) deserves equal attention. Viewing these two metrics together provides a complete picture. The oxygen reading is the available fuel; the pulse rate is how hard the engine is revving to distribute it.
The body has a built-in safety mechanism: when oxygen levels drop, the heart compensates by beating faster. A "normal" oxygen reading of 96% accompanied by a racing resting heart rate (e.g., 110 bpm) signals your body is working overtime. Recognizing this compensation can alert you to respiratory stress before saturation numbers fall.
The Blood Connection: How Hemoglobin Levels Influence Your Reading
A pulse oximeter determines what percentage of your "delivery trucks" (hemoglobin) are full. However, it cannot tell you the size of your fleet. If you have anemia (low hemoglobin), your device might report 100% saturation because the few red blood cells you have are fully oxygenated. Yet, your organs might still be starving for air because the total volume of oxygen is too low.
Because numbers can mask reality, trust your physical sensations. If you have conditions like anemia, watch for fatigue, pale skin, or shortness of breath even if your SpO₂ looks perfect.
Reading the Rhythm: What the Plethysmogram Wave Tells Your Doctor
The moving line scrolling across the display, known as the plethysmogram wave, acts as a visual confidence check. Before trusting the oxygen percentage, verify the machine is "hearing" your heartbeat clearly.
A healthy signal resembles a steady mountain range, with peaks rising and falling in sync with your heartbeat. This confirms blood is flowing strongly and the sensor is picking it up without interference. If the line looks like a jagged scribble or is flat, the device is struggling to find a pulse. In this scenario, any SpO₂ number displayed is likely inaccurate. Warming your hands or resting your arm can often smooth out the line.
Staying Safe at Heights: Oximetry for Hikers and Athletes
At high altitudes, air pressure drops, leaving fewer oxygen molecules for your lungs. Saturation levels naturally dip below the standard "sea level" range, often hovering safely between 88% and 92%. Understanding this prevents panic when numbers don't match what you see at home.
Successful tracking in these environments focuses on trends. While numbers drop during a climb, they should rebound when you rest, proving your body is acclimatizing. If the percentage fails to bounce back, it is a warning to stop ascending.
Medical Grade vs. Consumer Devices: Which One Do You Really Need?
The distinction between devices often lies in the label. An oximeter marked strictly for "sports and aviation" is a consumer-grade product. These work well for healthy people but are essentially "best guess" machines. Medical-grade devices must prove to the FDA that they remain accurate even when blood flow is weak or oxygen levels drop---exactly when you need them most.
If monitoring an illness, verify the device meets specific health needs:
- FDA Clearance: Look for "Class II Medical Device" or a 510(k) number.
- Accuracy Claims: Medical units guarantee ±2% accuracy.
- Signal Strength: Better units display a Perfusion Index.
Smart Shopping: Understanding Prices and Features
Finding the right balance between cost and quality depends on your needs. In global markets, prices fluctuate based on display technology and build quality. It is often worth investing in a device with a multi-directional OLED screen, which remains legible in dim lighting.
Your lifestyle dictates the sensor type. Most users only need a standard "spot-check" device. However, if you need to track oxygen levels while sleeping to screen for apnea, investigate wearable monitors that record data over several hours. While Bluetooth connectivity offers convenient logging, a customizable audio alarm on the machine itself is often a more critical safety feature.
Troubleshooting Guide: Fixing Jumpiness and Error Messages
Since a fingertip oximeter relies on light, tiny obstructions like dust or skin oils can block the sensor. A quick wipe with a cotton swab dipped in rubbing alcohol often clears the path. Inconsistent numbers also point to power struggles; weak batteries may light the screen but lack the energy to push infrared light through the finger. Always use fresh batteries if the readout seems erratic.
Ambient light interference from direct sunlight or bright lamps can also confuse the sensor. Simply cupping your hand over the device to create a shadow can instantly stabilize the data.
Your Oxygen Action Plan: Turning Data into Better Health Decisions
That small digital screen is no longer just a source of flashing numbers; it is a reliable fuel gauge for your body. By understanding how this technology works, you have transformed medical equipment into a tool for empowerment. You now realize that cold hands or movement are barriers that stop the sensor from seeing clearly, not just minor inconveniences.
This knowledge transforms your monitor from a reactive measure into a proactive tool. To turn this understanding into a safety net, implement this strategy:
- Establish your baseline: Measure levels when you feel well to understand what is normal for you.
- Optimize readiness: Keep the oximeter in your first-aid kit with fresh batteries.
- Prepare communication: Keep a log with your baseline numbers and your doctor's contact info ready.
Owning your health data allows you to advocate for your well-being. By combining your understanding of these sensors with a consistent approach to monitoring, you ensure you are always ready to listen when your body speaks.
Q&A
Question: What does SpO2 actually measure, and how is it different from pulse rate?
Short answer: SpO2 (oxygen saturation) tells you how fully loaded your red blood cells are with oxygen—the quality of the “fuel” reaching your organs. Pulse rate (PR/BPM) measures how fast your heart is beating—the speed of the “engine.” You can have a normal heart rate while your oxygen is low, or a normal SpO2 while your heart is racing to compensate. Looking at both together gives a fuller picture: SpO2 shows supply, PR shows effort.
Question: What readings are normal, and when should I worry or seek care?
Short answer: For most healthy adults, 95%–100% is normal. If you see 91%–94%, reassess how you feel and consider contacting your healthcare provider, especially if you’re ill or short of breath. At 90% or below, seek immediate medical attention. Baselines vary—people with COPD may have a safe range set by their doctor (often 88%–92%). Focus on trends rather than one-off dips, since posture, movement, or cold hands can momentarily lower the number.
Question: How do I get a reliable home reading, and what causes false lows?
Short answer: For accuracy, use this 5-step routine: rest 5 minutes, warm your hands, keep your hand at heart level, stay still with the clip on your middle or index finger, and wait ~30 seconds for stabilization. False lows often come from cold fingers (poor blood flow), dark nail polish blocking light, bright ambient light, low batteries, or a loose fit. Remove polish or rotate the clip, warm your hands, shield the sensor from bright light, clean the LEDs, and retest calmly.
Question: How does a pulse oximeter work, and what do PI and the plethysmogram wave mean?
Short answer: The device shines red and infrared light through your fingertip. Oxygen-rich hemoglobin absorbs more infrared and lets more red pass; oxygen-poor blood does the opposite. By comparing light absorption, it estimates your SpO2. The Perfusion Index (PI) reflects signal strength at the finger—very low PI (e.g., <0.4) means the sensor is struggling, while values above ~0.2 usually indicate a usable signal. The plethysmogram (scrolling pulse wave) should look like steady, rhythmic peaks; a jagged or flat line suggests the device isn’t detecting a clean pulse, so reposition, warm up, or reduce motion before trusting the number.
Question: Which oximeter should I buy—and do I need a medical-grade model?
Short answer: Match the device to your needs: fingertip units are portable for spot checks, handheld models offer better stability for caregiving, and tabletop/ICU units enable continuous monitoring with alarms. For illness monitoring, look for medical-grade features: FDA clearance (Class II/510(k)), stated ±2% accuracy, and a displayed PI. Consider an OLED screen for readability and on-device alarms for safety; Bluetooth is optional. For children, use pediatric sensors designed for small fingers and higher heart rates to avoid erratic readings.